In contrast to the predominantly bony hip joint, the knee joint is a capsule-ligament-guided joint. The two cruciate ligaments located centrally in the knee joint, along with the collateral ligaments and other capsular ligaments, are the most important stabilizers of the knee joint. They are called cruciate ligaments because their course crosses over in the joint and, from a biomechanical point of view, they form an "overlapping joint chain". In this way, the cruciate ligaments ensure the "roll-slide mechanism" in the knee joint, which guarantees flexion and extension of the knee joint in the same plane of movement at all times.
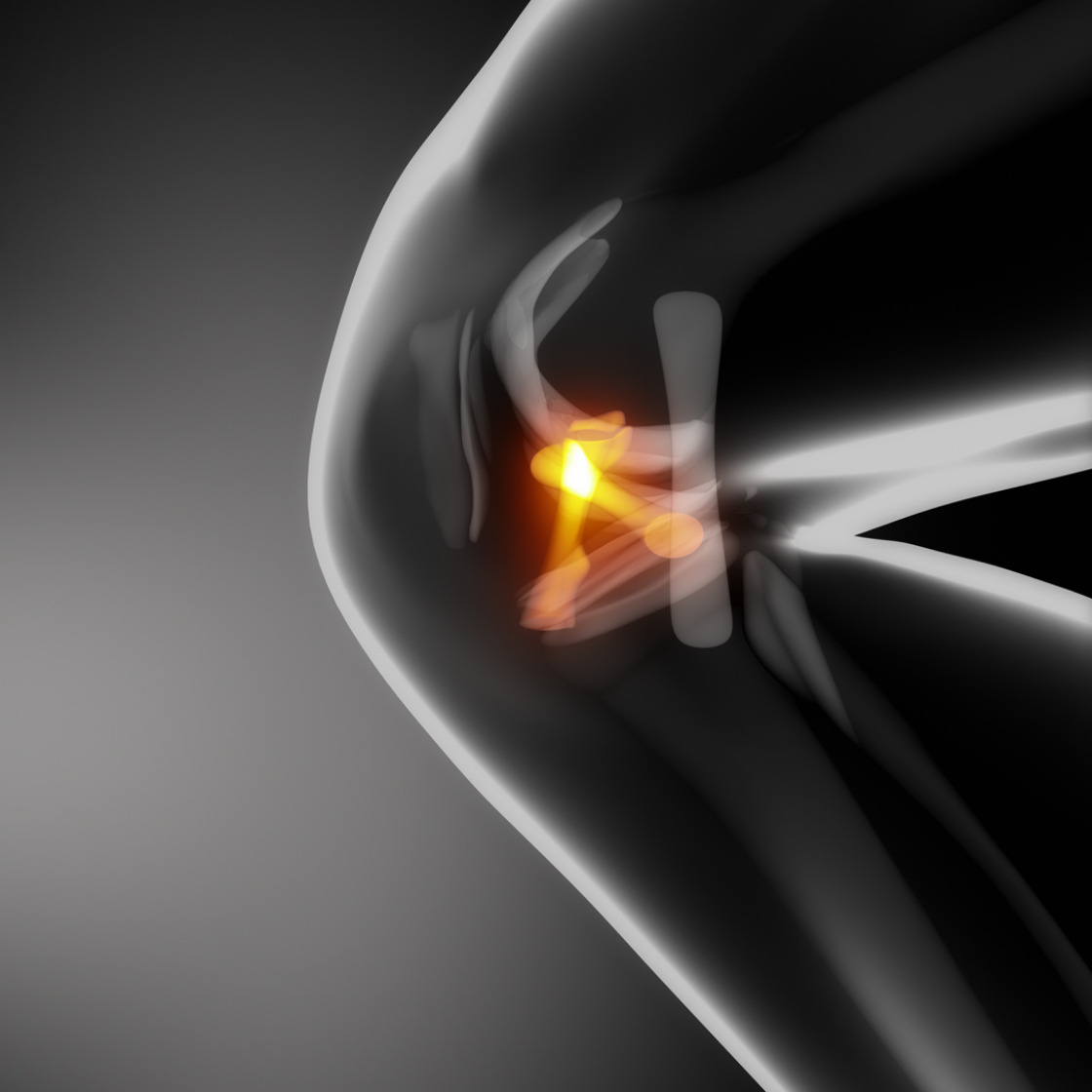
In recent years, there has been a significant increase in capsular ligament lesions of the knee joint (about 80 per 100,000 inhabitants according to Swiss accident statistics). In about 65% of cases, sports accidents are responsible for knee ligament injuries, especially contact or accelerated sports such as soccer, handball or skiing.
Among ligament injuries, anterior cruciate ligament injury is the most common, accounting for about 45%, followed by isolated injury to the medial ligament, and then anterior cruciate ligament rupture combined with rupture of the medial ligament and / or medial meniscus. In contrast, the posterior cruciate ligament is very rarely injured. We see most anterior cruciate ligament injuries as a result of deceleration twisting trauma of the knee joint without external impact.
Patients typically describe a feeling of instability and many hear or feel a crack at the time of injury. After the injury, the patient typically cannot continue playing and the knee joint often swells within a short period of time. In contrast, swelling from a meniscal injury or osteoarthritis overload takes 1-2 days to develop.

The anterior cruciate ligament (ACL) stabilizes the lower leg against forward displacement, the posterior cruciate ligament stabilizes it backward. The absence (tear of the cruciate ligament) causes instability (wobbly knee). Even during normal walking, this instability leads to abnormal displacement movements between the joint surfaces of the upper and lower leg, which in the long run leads to meniscus damage, widespread ligament loosening and increased cartilage wear, which then eventually results in wear (arthrosis).
These shifting movements have an even more unfavorable effect under further athletic strain.
The consequence is even earlier damage to the joint structures mentioned above, even in younger people. To avoid this late damage, the anterior cruciate ligament should therefore be replaced. In this case, suturing the anterior cruciate ligament has not proven to be a successful method because of the poor blood supply to the ligament, and replacing a cruciate ligament with an artificial ligament has not proven to be a successful method because of the strong mechanical load cycles.
Therefore, the current treatment of choice is the replacement of the anterior cruciate ligament with autologous material, which is then referred to as "autologous anterior cruciate ligament reconstruction".
The anterior cruciate ligament (ACL) stabilizes the lower leg against forward displacement, the posterior cruciate ligament stabilizes it backward. The absence (tear of the cruciate ligament) causes instability (wobbly knee). Even during normal walking, this instability leads to abnormal displacement movements between the joint surfaces of the upper and lower leg, which in the long run leads to meniscus damage, widespread ligament loosening and increased cartilage wear, which then eventually results in wear (arthrosis).
These shifting movements have an even more unfavorable effect under further athletic strain.
The consequence is even earlier damage to the joint structures mentioned above, even in younger people. To avoid this late damage, the anterior cruciate ligament should therefore be replaced. In this case, suturing the anterior cruciate ligament has not proven to be a successful method because of the poor blood supply to the ligament, and replacing a cruciate ligament with an artificial ligament has not proven to be a successful method because of the strong mechanical load cycles.
Therefore, the current treatment of choice is the replacement of the anterior cruciate ligament with autologous material, which is then referred to as "autologous anterior cruciate ligament reconstruction".
The semitendinosus and gracilis tendons belong to an anatomical structure consisting of four muscles and tendons on the inner side of the thigh. One (semitendinosus tendon) or even two (gracilis tendon) tendons are taken from this package via a small skin incision and arthroscopically retracted into the knee joint as a triple or quadruple layered bundle via a drill channel at the tibial head and then fixed "isometrically", i.e. at their anatomical points in the femur and sliding head. Fixation is achieved by means of biodegradable clamping screws, transverse dowels or by a small metal plate on the femur. The material therefore does not need to be removed later.
The advantages of this method are the low removal pain after the operation and the unimpaired stretching and kneeling ability of the joint.
The patellar ligament is approx. 25 mm wide. From this, an approx. 10 mm wide central tendon strip with a bone block each can be removed from the tendon insertion at the patella and at the tibial plateau and then also fixed arthroscopically in the joint via drill channels with clamping screws. The advantages here are the very good primary stability due to the fixation of bone to bone. Disadvantages are pain, which can occur at the removal site, a possible reduction in muscle strength during extension of the knee joint, as well as the principle risk (very rare!!) of a tear of the remaining patellar tendon or a patellar fracture.
The surgical techniques described above allow rapid (partial) loading and freedom of movement of the knee joint. A knee guide splint (orthosis) is often prescribed for the first 4 - 6 weeks after surgery. The physiotherapeutic aftercare improves the movement of the knee joint in the beginning, then, after an increase of the muscle strength, the promotion of the coordination follows and finally the quick strength training. All in all, rehabilitation after anterior cruciate ligament surgery takes several months, with contact and accelerated sports prohibited for at least 6 months. With accurate surgical technique, consistent physiotherapy and motivation of the patient, they usually regain their old sports activity level.

December 22 + 23, 2025:
Dortmund practice closed.
The practices in Datteln, Recklinghausen, and Kamen are open.
December 24 – 26, 2025:
All practices closed.
December 29, 2025 + December 30, 2025:
Datteln and Kamen practices closed.
The practices in Recklinghausen and Dortmund are open.
December 31, 2025 – January 2, 2025:
All practices are closed.
Outside our office hours and in urgent emergencies, please contact the medical emergency service at: 116117
The entire team at Cureon Clinics ONZ wishes you
a peaceful Christmas season.
